Declining Predictive Power of Medical Underwriting
We are living through unprecedented times. Some of us are adjusting and adapting but many lives have changed drastically.
In our industry - life and health insurance - disruption was inevitable. We are all aware now that there is only a slight impact from increased losses as mortality rates remain within loss thresholds. The big impact will come from disruption in financial markets eroding investment returns but at the same time it will probably drive sales as people feel a lot more vulnerable.
This will put further pressure on insurers to increase their reach and improve the customer buying experience - especially health risk assessments. Due to social restrictions, in the short run, optimising the online direct-to-customer channel is an absolute necessity. However, until health assessments rely on tons of personal and health questions and medical exams customers will continue to drop out..
Today most insurers use mortality tables developed in the late part of the 20th century, historical trends and risk groupings (age, gender, occupation, family history) to predict health and mortality outcomes for pricing protection products. The amount of information required and the constant back-and-forth for clarifications and exceptions results in a customer journey spanning weeks on average.
Diminishing Predictive Ability
The basic (age, gender) models achieve accuracy, measured by area-under-the-curve (AUC) of around ~ 80%. Some additional variables assessed do have high correlations with mortality but over time they have exhausted their ability to differentiate beyond broad classification buckets.
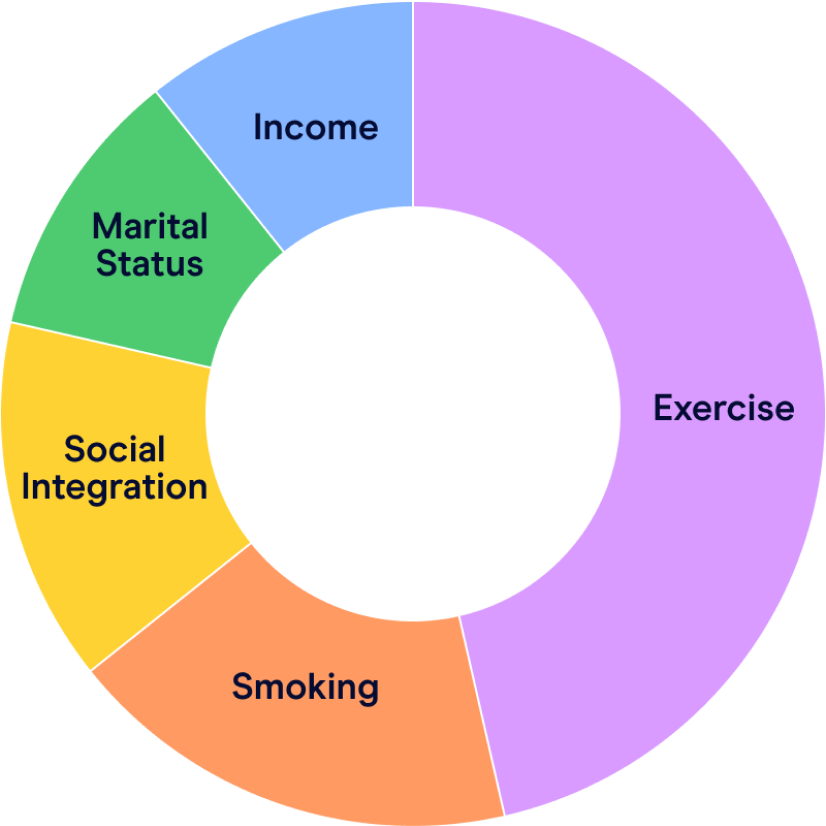
There’s plenty of research examining this challenge. One multi-country study published in PLOS measured improvement in accuracy for 57 predictors. Contributions of the top predictors are as follows:
Other than ‘smoking status’ none of the other predictors are assessed under traditional underwriting, either due to lack of data availability or regulatory restrictions resulting in most of the loading weightage derived from Age and BMI.
Personal Responsibility and Individual Agency
Another problem with the traditional approach is that it doesn’t reward improvements in health. It doesn’t acknowledge customer’s agency to improve their wellbeing. Exercise and mobility reduce risk of major health conditions and mortality and enhance immunity to emerging risks.
What’s relevant here is that, other than better risk selection and customer experience, for a long time insurance companies have known, that higher returns lie in prevention and health improvements of the customers. At a time when sense of personal responsibility will define national health outcomes across countries there is a big opportunity for insurers to incentivise behaviour and empower individuals to build healthier and more resilient societies.
Conclusion
Better risk classification and pricing differentiation are proven strategies to increase sales and margins. These also pose threats as challengers, free from legacy, are rebuilding predictive models for the future. For example, along with using the most significant predictors our algorithm is trained on real-life data sets of highly representative populations which allows us to translate risk scores to extra-morbidity and extra-mortality risks for the target markets.
The disruption brought about by the virus outbreak has prioritised remote engagement, digital risk assessment and emerging data sources as agent/broker channels are suspended and medical exams cannot be conducted. Ability to overcome these challenges in the short-term and realigning the value proposition for the future will result in the biggest wins and losses.
References:
Actuarial Post
PLOS
Harvard Health
McKinsey



